Written by
Chloe Garnham
Content warning
This article references potential trauma triggers, including disordered eating, depression, anxiety, PTSD, self-harm, and suicide. If you are in distress and need immediate help, trained counselors are available to take your call. Please find a crisis hotline in your country here.
Hunger cues are powerful signals that motivate you to eat and govern dozens of food-related decisions you make every day.
For many people, eating or thinking about food is pleasurable. However, for some, it causes feelings of anxiety and stress that contribute to unhealthy eating patterns. What, how, and when we eat depends on a wide variety of psychological, social, environmental, economic, and cultural factors.
Fortunately, there are ways to identify harmful patterns regarding food and develop healthier approaches to eating. However, it’s also essential to recognize the signs that indicate unbalanced eating behaviors require help from a qualified healthcare professional.
Disordered eating or eating disorder?
Though many use the terms interchangeably, disordered eating and having an eating disorder are two distinct things. Disordered eating is not necessarily an eating disorder. The term itself is not a diagnosis. Instead, disordered eating is a way to describe irregular eating behaviors — some of which will fall into the much narrower definition of an eating disorder.
An eating disorder is a clinical diagnosis defined by the American Psychiatric Association, and it falls into one or more separate categories:
- Anorexia nervosa (AN)
- Bulimia nervosa (BN)
- Binge eating disorder (BED)
If you visualize all eating behaviors existing on a spectrum of healthful to harmful, one end is being tuned into whether you’re hungry or satisfied — so-called “normal” eating.
The other end would represent having an eating disorder, a form of mental illness relating to eating behavior, body image, and weight.
Disordered eating would land in the middle, representing an unbalanced or, in some ways, dysfunctional relationship with food.
An eating disorder is disordered eating at an extreme.
Many more people are affected by disordered eating than an eating disorder. Still, just because unhealthy eating patterns don’t fit the criteria of a disorder, doesn’t mean they don’t need to be taken seriously.
All concerns about eating, clinically disordered or not, deserve proper attention and support.
What are the signs of disordered eating?
Disordered eating patterns show up differently from person to person. However, some of the common signs and symptoms include (but are not necessarily limited to):
- Basing self-worth mainly on body shape and weight
- Being in a healthy weight range yet believing you’re overweight
- Exercising excessively or very rigidly
- Having feelings of guilt and shame to do with eating
- Counting calories obsessively
- Only eating certain foods or being inflexible about when you eat
- Feeling a loss of control or compulsion about eating habits
- Refusing to eat outside of your home (such as in restaurants)
- Being preoccupied with your body and food to the point that it interferes with your enjoyment of life
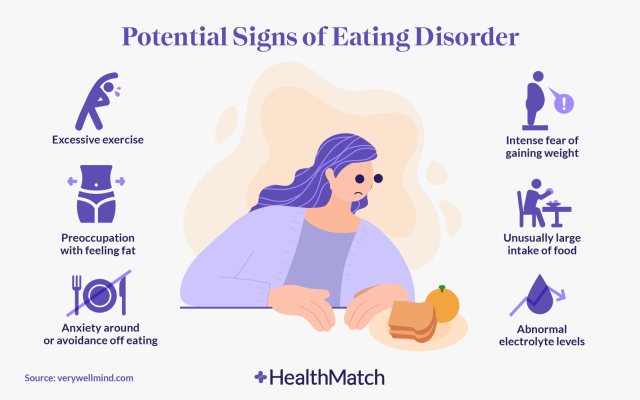
Disordered eating potential red flags
Disordered eating raises your risk for a wide variety of health complications, such as developing anxiety and depression.
An imbalanced relationship with eating can also elevate the risk of being overweight or underweight, having issues with your blood pressure, bone density, heart rate, digestion, and fertility.
If you recognize that you or someone you care about exhibits any red flags related to eating, please seek help from a qualified healthcare professional. If you want to connect with a trained counselor, find a toll-free crisis hotline in your area here.
Restricting food
Restrictive eating is a broad term that includes a range of restrictive eating patterns. These patterns can be damaging both psychologically and physically, especially if an individual is continually undereating.
Symptoms of restrictive eating can include obsessive calorie tracking, refusing to eat certain foods, eating smaller portions than the body requires, or deeming certain foods as “good,” “bad,” or “off-limits.” There may also be intense anxiety about food or feeling the need to skip meals, fast for long periods of time, or limit food intake.
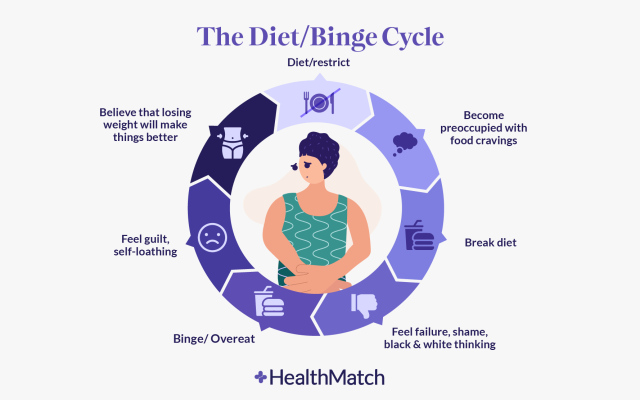
Binging-purging cycle
A common symptom of bulimia (binge eating and purging) involves consuming large amounts or large calories of food within a short period of time, even when not hungry. Binge eating can, in some cases, occur as a result of restrictive eating.
After limiting food intake for a long period of time, a person will become so hungry that they binge eat, then self-induce vomiting. This behavior is frequently associated with feelings of losing control, shame, sadness, and inabilit to stop oneself from eating.
Emotional eating
Eating for emotional reasons is another unhelpful eating behavior, especially when you aren’t hungry or when you’re full. This might happen due to stress, anxiety, or boredom. Emotional hunger tends to happen suddenly rather than gradually.
Having a physically full stomach doesn’t always factor into behavior during episodes of emotional eating. Specific foods and cravings may be involved, and the experience may trigger feelings of guilt, shame, and powerlessness.
Over-exercising
For individuals who tend to overeat, or eat emotionally, exercise can be an essential way to improve physical health and boost mood. However, over-exercising can be equally problematic.
Those with disordered eating — especially individuals who restrict food — may experience a compulsion to exercise and engage in excessive physical activity, resulting in unhealthy weight loss and being underweight.
A 2017 study¹, Compulsive Exercise: Links, Risks, and Challenges Faced, found that the most common negative consequences of excessive and compulsive exercise included injuries, social impairment, and depression.
Are eating disorders on the rise?
Bringing together all the relevant data about eating disorders is incredibly complex. However, the findings of a 2019 systematic literature review² published in the American Journal of Clinical Nutrition do point to a rise in prevalence.³ The authors found that global rates of eating disorders have risen from affecting 3.5% of the population between 2000–2006 to 7.8% during 2013–2018. That same review analyzed 121 different studies but doesn’t reflect growth data on disordered eating patterns (individuals who don’t meet the clinical criteria for an eating disorder but still struggle with unhelpful eating behaviors). So, disordered eating may be an even larger public health concern than adequately captured.
Similarly, in another study, researchers found that although anorexia and bulimia are included in the Global Burden of Diseases, Injuries, and Risk Factors Study 2019, binge-eating disorders and other specified feeding or eating disorder (OSFED) are not. Yet binge-eating disorders and OSFED are more prevalent and account for an additional 41.9 million cases worldwide. This finding suggests a need to include additional disorders for a more complete picture of eating disorder data and trends.⁴
Who is most at risk?
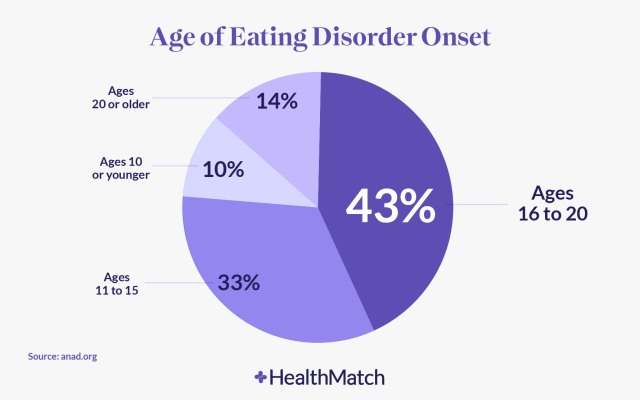
Those who identify as women and girls are disproportionately impacted by irregular eating behaviors and clinical eating disorders, though there is a growing public awareness that males are affected too.
According to the National Eating Disorders Association, females between ages 12–35 are at the highest risk of experiencing disorders related to eating.⁵ One study investigating the patterns and prevalence of disordered eating in 4,023 female participants ages 25–45 found that even women without an eating disorder had “unhealthy approaches to weight control and negative attitudes about shape and weight.”³ In the same study, 74.5% of respondents reported concerns about body shape and weight that interfered with their happiness. Another study found that throughout their lifetime, 4% of females and 0.3% of males experience anorexia nervosa (a condition involving unwarranted fear of being overweight). 3% of females and 1% of males experienced bulimia nervosa (a condition involving binging and purging food).⁶
A literature review comparing the prevalence of eating disorders in Western and Non-Western Countries found fewer cases of eating disorders in non-Western countries, but that number appears to be rising.⁷ The authors hypothesize that urbanization and westernization are at least partly to blame.
Unique challenges presented by the COVID-19 pandemic
The pandemic has hurt eating habits. For example, a survey from the British Nutrition Foundation found that the pandemic encouraged unhealthy eating habits.⁸ 27% of adults surveyed felt that they were eating less healthy during lockdowns, mainly due to boredom, stress, anxiety, and tiredness. In addition, 30% couldn’t go to the store as often which they felt led to them eating less healthily.

The connection with other mental and physical illnesses
Eating disorders are commonly linked with other health issues. Research has found that 56-95% of individuals diagnosed with eating disorders are also diagnosed with one (or more) additional physical or mental health conditions.⁹
Commonly, eating disorders are associated with mood disorders including major depressive disorder, post-traumatic stress disorder (PTSD), anxiety disorders (including OCD and social anxieties), sexual dysfunction, self-harm, and thoughts about suicide.¹⁰
These data highlight the critical need for integrated treatment that goes beyond the physical requirement of proper nutrition.

Four steps to addressing disordered eating
Overcoming disordered eating can be challenging, especially since long-held habits may be involved. Individuals who experience disordered eating often have a skewed body image, making it particularly crucial to seek outside support and professional help. Here are some steps you can take if you believe that you or someone you care about have disordered eating patterns:
1. Get professional medical advice
A doctor can diagnose both disordered eating and a specific eating disorder. They may also provide helpful information, support, or a referral to a registered dietitian, psychologist, or a similarly trained professional.
2. Speak to a mental health expert
Disordered eating is a psychological condition, and it’s common for other forms of mental illnesses like anxiety and depression to also be present. So, it’s particularly important to connect with a mental health professional to ensure that all your needs are being considered and addressed in your treatment plan.
3. Work with a registered dietitian
Working with a registered dietitian or nutritionist experienced in treating disordered eating is an important way to make sure that advice, meal plans, and counseling are all relevant to your condition. You may be unaware of certain unhelpful habits because they’ve become second nature. A dietitian can help you identify these behaviors and assist you in developing strategies for maintaining healthy eating patterns.
Some of the topics you may work with a dietitian on include:
- Understanding the importance of nutrition
- Recognizing restrictive behaviors and how they can negatively affect your health
- Establishing a healthy weight
- Adopting tools to avoid unhealthy dieting or binging habits
- Developing healthy, regular eating patterns
4. Learn about eating mindfully
In our fast-paced, modern world, eating can feel purely functional at times — you might quickly eat breakfast before dashing to work or school, or eat mindlessly in front of the TV. However, you’re not just throwing fuel in the tank of your car, you’re taking care of your health. If you don’t eat mindfully, it’s easy to lose track of how fast or how much you’ve eaten. Eating with greater intention can be helpful, especially if you tend to binge eat or eat emotionally.
Some useful ways to bring mindfulness to mealtimes include:
- Eating slowly without distractions like your phone or television
- Learning to recognize hunger cues to help notice the difference between being hungry, bored, or stressed
- Becoming more aware of fullness signals to avoid overeating
Tips for maintaining a healthy weight
If you experience disordered eating, it may be challenging to recognize whether it would be healthful for you to gain or lose weight. Some individuals may have a distorted view of their body and weight level. Above all, talk to your doctor about your weight concerns so you can get their guidance.
If your doctor thinks that weight gain or weight loss would be beneficial, the following tips may help you along the way
- Reduce stress and anxiety by focusing on eating to nourish your body, not just to lose or gain weight.
- Eat sufficient calories and volume at mealtimes to avoid undereating or binging.
- Plan for gradual, sustained change. Don’t expect your weight to shift overnight.
- Meal planning, eating regular meals, and having nutrient-dense foods on hand for snacks are all helpful.
- Work with a dietitian to map out attainable behaviors that work with your daily routine.
The lowdown
Disordered eating is a widespread issue affecting millions of individuals around the globe. Those who have unhealthy eating patterns may or may not fit the clinical criteria for an eating disorder. However, all unhelpful habits around food and eating warrant help, especially if they cause distress. When ignored, disordered eating can seriously impact both mental and physical well-being and can even be fatal in some cases. While experiencing disordered eating can make those affected feel powerless, the condition is treatable. There are many strategies to help, and returning to healthy eating is possible with the proper support. The most crucial step is to reach out and talk with a qualified doctor or healthcare provider.
The information provided is designed to support, not replace, the relationship that exists between a patient/site visitor and their existing health care professional(s).
Have feedback? Send an email to [email protected].
Sources:
- Compulsive exercise: links, risks and challenges faced (2017)
- Prevalence of eating disorders over the 2000–2018 period: a systematic literature review (2019)
- Patterns and prevalence of disordered eating and weight control behaviors in women ages 25-45 (2009)
- The hidden burden of eating disorders: an extension of estimates from the global burden of disease study 2019 (2021)
- Statistics & research on eating disorders | National Eating Disorders Association
- Incidence, prevalence and mortality of anorexia nervosa and bulimia nervosa (2021)
- Prevalence of eating disorders: A comparison of western and non-western countries (2004)
- British nutrition foundation healthy eating week 2020 – insights into the effect of COVID‐19 on eating and activity habits of adults and children in the UK (2021)
- Comorbid eating disorders in persons with other mental illnesses (2020)
- Changing the course of comorbid eating disorders and depression: what is the role of public health interventions in targeting shared risk factors? (2014)
General sources:
- Eating behavior – Encyclopedia of behavioral medicine (2013)
- What is disordered eating? | Eat Right
- Anorexia nervosa | National Eating Disorders Association
- Epidemiology of eating disorders: Incidence, prevalence and mortality rates (2012)
Chloe Garnham is a writer exploring a broad range of topics, including healthcare, education, and technology.